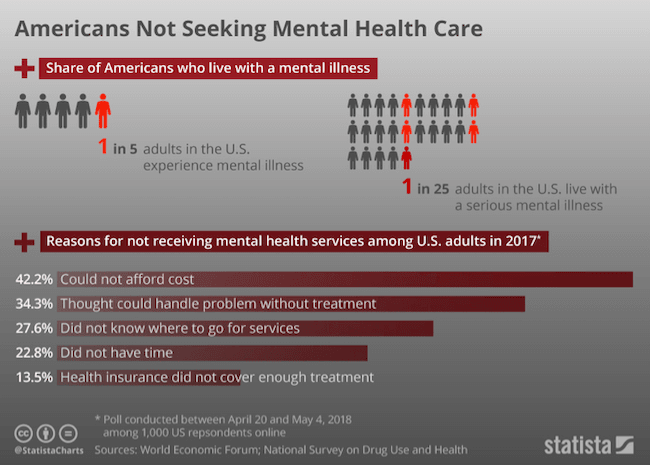
These are the ugly, dark parts of mental illness and drug addiction that no one talks about, and by not talking about it, it stays hidden, and shameful, and powerful, and deadly.
My sister had 765 “friends” on Facebook. I don’t think I even know that many people. But I can count on one hand how many of those friends came to visit my sister during her four-month hospital stay. So apparently they were friends, but not quite that close.
I believe that if regret had a smell, it would be the smell of something burnt and visceral, and sharp in your nostrils. I think of that every time I listen to the last voicemail that my sister left me. It was so normal, absolutely nothing special about it, like the countless other messages we had left each other.
“Hi baby girl, it’s me. Call me back. Love you.”
Sometimes I listen to it just so that I can hear her voice, but often I find myself straining to hear something that I must have missed. Did she know that she was dying? Was there some sort of resolve in her voice? Or was that loneliness? But mostly what I hear is regret. Mine, of course, not hers. Because no matter how much I loved her, I couldn’t save her. I am painfully aware that I failed my sister. Sometimes I think that we all did.
Malika and I were two years and 10 months apart, and about as different as two people carved from the same parents can be. She was always the pretty one, the free spirit, and she had the goofiest sense of humor. The boys simply didn’t see me when we were together—she shone that brightly—and we could fight like nobody’s business. But above all, she was amazing to me.
My sister was diagnosed with bipolar disorder and schizophrenia in high school, which apparently is a common age for that to rear its ugly head. We both shared a sort of rebellious streak borne out of a sometimes-tumultuous home life and an ugly divorce between our parents, but she never really grew out of hers. She had a self-destructive side but it was always directed inwards—she never set out to hurt anyone but herself. I can see clearly now that for years, she was self-medicating.
There were many times over the last few years that I had no way of getting hold of her. She often changed her phone number, and she and her boyfriend moved around a lot, either by choice or necessity. That was the thing about my sister: when she was healthy enough and able to be around people, she was great. Absolutely great. But often, and particularly in the last several years, when she didn’t want to be found, she went completely off the grid. I had heard rumors that at one point she was seen in the city begging for money for drugs. Another time I heard she was staying in the house we had grown up in while it was empty and in foreclosure.
I ask myself all the time what I could have done differently, or what I should have done. But you cannot save someone who doesn’t want to be saved, and you certainly can’t force them to get help. If you give them money, you know where it’s going to end up, but do you do it anyway? I’ve been on both sides of this, and I know that you’re damned if you do and damned if you don’t. And when you don’t, they hate you and disappear again—proving that it was the only reason they resurfaced in the first place.
I don’t even know how many times my sister tried rehab over the years. I do know that she tried. She had been in a day treatment program and was on methadone when she was admitted to the hospital last August. She was confused, bloated, and had no idea where or who she was, and she didn’t recognize me when I first came to see her. She had every drug you can think of in her bloodstream. They said that the confusion was caused by a bacterial abscess on her cervical spine just below her brain that had developed from repeated IV drug use with a dirty needle, and they started treating her on a wide spectrum of antibiotics. About a week in, she started coughing up blood and spiked a fever. Despite being on so many antibiotics, the infection in her bloodstream had attached itself to a valve in her heart, and every time her heart beat, it scattered more of the infection throughout her bloodstream. She slipped into a coma at that point and ran a fever that ended up lasting for weeks.
Watching her go through that was a special kind of hell, wondering if she was ever going to wake up. She went in and out of consciousness and agitation as the doctors wrote things down like acute respiratory distress (ARDS), MRSA, MMSA, endocarditis, pneumonia, and acute pulmonary edema. All the while her fever kept climbing and I sat with her completely helpless, watching the numbers climb and her cooling blanket sweating into a puddle on the floor. Eventually they had to do a tracheostomy because she wasn’t breathing properly on her own.
At the end of October, they finally managed to keep her fever below 100 degrees for a full 48-hour window and were able to take her into surgery to replace the heart valve that by now had been completely destroyed. The surgeon very kindly and very gently told me to prepare for the worst because even in a very healthy patient, open heart surgery brings significant risks. In Malika’s severely compromised state, the odds were not at all good that she’d wake up from surgery.
But true to form and consistent with her defiant and rebellious spirit, she did. Amazingly, I began seeing my sister come back to me. Despite all the odds, she started to bounce back and gradually brought her spunky personality and wicked sense of humor with her. I’ll never forget the day I walked into her room and she simply smiled and said “Hi Shawn,” like it was no big deal. I remember that I actually stopped walking and that when I tried to speak, I was so caught off guard that it came out in a strangled sob; just that morning, she was finally improving enough that the doctors were able to take her trach out, and she was able to speak for the first time in I don’t even know how many weeks.
I wish I could say at this point that her story became a fairy tale and she walked out of the hospital and into a brand new life with the second chance she was given. But addiction is not all sunshine and roses. The truth is, the better she got, the more she simply wanted out, and all the talks we had about rehab gradually fell away. She made up her mind that she was fine and just wanted to be free of all the IVs and round-the-clock medical care. What everyone involved in her treatment overlooked was that during the entire four months she was hospitalized, there were no concrete plans being made for her recovery, no drug treatment, no 12-step program, nothing to work on the addiction that had been slowly killing her since we were teenagers.
This realization fully hit me for the first time when she was caught by one of her nurses trying to drink the alcohol gel beads inside one of her ice packs. The nurse told me that she had been asking for them on a regular basis and had apparently been hoarding them for just this purpose. Up until that moment, I’d never understood why they took away perfumes and mouthwash and anything else with even trace amounts of alcohol when you check into rehab. Malika was not clean or sober during those four months she was hospitalized. She was simply separated from her addiction.
Which is why, after seeing her nearly every day for those four months that she was in the hospital, she quietly pulled away from me after she was discharged at the end of December. She never did check into the rehab or residential facility that she promised she’d go to when she got out. Gradually, she stopped returning my calls and texts.
So I wasn’t that surprised when the hospital called on May 25, 2018, just five months later, to tell me my sister was admitted back into the ICU and that, as her healthcare proxy, they needed my consent to treat her since she was wasn’t coherent. This time, the doctor said that the spots on her arms were a sign of heart failure, and an MRI showed that the confusion was caused by scattered spots of bacteria throughout her brain. That beautiful, robust new heart valve that had given her a glorious second chance at living just a few months before was now infected from a dirty needle again. And when the doctor said that her fever this time upon admission was 109 degrees, I was sure I heard him wrong. I didn’t even know that was possible, and that was while she was wrapped in a cooling blanket. They watched her around the clock for seizures and told me she would likely have brain damage when she woke up. When her fever finally broke and she came to a couple days later, I remember thinking that the light in her eyes had dimmed. She never really bounced back this time.
When I went up for my daily visit with her at lunchtime on June 5th, we had one of the best visits we’d had in months. I remember very clearly telling her how much I loved her hair short, and how she was sitting on the side of her bed swinging her feet like a little kid. I remember her telling me that she was so sick of being in the hospital and that there was never anything good on television. But for the life of me, I cannot remember how we ended that visit. Every single time I left the hospital after spending time with her—every single time—she made me promise that I’d come back to see her. And I’d always laugh and tell her of course I would, I always do. It had almost become a ritual: I knew she’d say it, childlike and sweet, and she knew exactly how I’d respond. Maybe it was reassuring to her and she just needed to hear it. Or maybe I just wanted to remind her that I’d always come back. But I have replayed our conversations from that day over and over and over again, and I cannot remember her asking me to make that promise to her on that afternoon, or what I said to her when I left. And it haunts me.
That night, just before midnight, I was woken by someone banging on the front door and the dog flipping out. My husband opened the door bleary-eyed. A friend of my mom’s stood there, frantic, saying that we had to come right away to the hospital; they had been trying to call me and couldn’t reach me. She said my sister’s heart had stopped and she was dying. I couldn’t comprehend her words. I told her I’d just seen my sister that afternoon and we had a great visit and she was fine. We don’t have time, she said. Just come.
When I grabbed my phone, I saw I had seven missed calls from the hospital. Seven. We got to the hospital in record time; a nurse was waiting for us and waved us to her room.
Malika died a few minutes before we got there. Minutes. I will always believe her death occurred after one of those seven calls, and that I was too late to save her, again. They told me that the overnight nurse came to check her vitals and found her in bed, unconscious with foam on her lips. They think she must have had a seizure, and her heart, which had already been through so much, finally gave out. One of the nurses rode the gurney doing CPR all the way up the elevator and into the intensive care unit, but they were never able to bring her back. She was 43.
Most of that night is a blur, stretched out unnaturally long in some places and disjointed and quick in others. But what I remember most clearly is the look on my sister’s face, and I carry that image with me, especially on the hardest days. I had come into her hospital room countless times when she was sleeping, and sometimes I just sat with her while she slept, while other times she woke up to talk with me for a while. But in all of those times, she kept this tiny wrinkle in her brow while she slept—like she was trying hard to remember something important. That night, though, that little wrinkle was gone, and she looked relaxed, peaceful, even. I realize that sounds so cliché, but it’s the only way I can describe it. She was finally, finally free of the demons she’d been running from for most of her adult life.
These are the ugly, dark parts of mental illness and drug addiction that no one talks about, and by not talking about it, it stays hidden, and shameful, and powerful, and deadly. And I am not ashamed of any of this—just unbearably sad for what my sister went though—and I am so angry at myself for not having done better. For not knowing what to do, or what she needed, and believing that she wanted me to stay at an arm’s length when she must have been in so much pain. In all the days since my sister passed, I’ve promised her that I would do something on her behalf, so that what she went through wasn’t in vain. I am still working on this.
But for now, I will continue to take my sons to the memorial bench that we bought for their Aunt Malika in the middle of a wildflower garden at a nature park near our first house, and I regularly talk to them about their goofball aunt who loved them more than life itself. I want to be sure they remember her at her best, while also understanding in no uncertain terms that if she could have beaten this horrific addiction, she would have, and she’d still be here to watch them grow up. I want to share her story because she was so much more than the addiction that claimed her life in a horrific and painful slow-motion free fall.
Malika was beautiful, wickedly smart, funny, kind, and free-spirited. I want people to remember her as the girl who followed Phish for a month one summer with her old boyfriend and their dog in a piece of crap van that they took across the country. Or the girl who wore her long, curly hair in pigtailed knots while she danced with my sons in the kitchen to Christmas songs in July and would do absolutely anything to make them laugh. Or the girl who could talk to and make friends with anyone, absolutely anyone, with ease.
It is that girl that I remember when I sit on her bench with the sun on my face and my eyes closed, remembering the sound of her laugh. I hope she knows how sorry I am that I didn’t do better for her, and how much I love her. And that even though I sat with her every day, I was ultimately no better than the 765 friends who did not. Because I didn’t know how to fix this.