When it comes to executing people by lethal injection, “Fentanyl is just an obvious choice. You have unfortunately an inexhaustible supply of this drug in state custody – why can’t it be used?”
As the end drew near, Carey Dean Moore’s face turned red, and then purple. He breathed heavily, according to the witnesses who were there to see it, and coughed. Roughly 20 minutes later, he died.
In his final weeks, the two-time killer had given up efforts to seek a reprieve. He’d expressed his scant apologies and written the final words condemned men write.
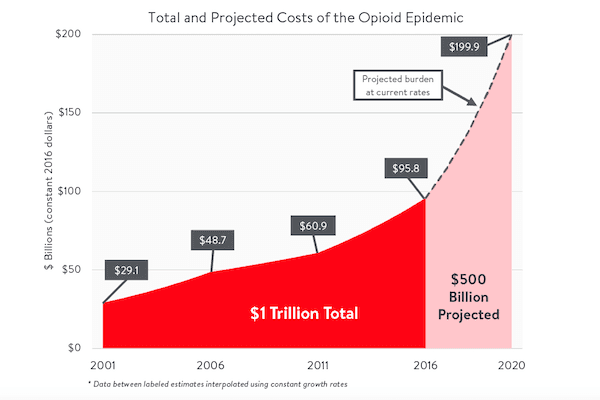
It was the 1,481st execution in the modern era of capital punishment, but Moore’s death was a first on more than one front. Not only was it the Cornhusker State’s first execution in more than two decades, but also it was the nation’s first ever lethal injection using fentanyl, the deadly drug at the center of the opioid crisis.
More than 28,000 Americans — none of whom were on death row — died in connection with the powerful painkiller in 2017, according to federal data.
Yet, as politicians and public advocates wrung their hands over how to stem the flow of drugs and stop the scourge of overdoses, behind closed doors corrections officials quietly asked a very different question: Can we use this drug in executions?
As long as it’s available, the answer is yes.
But as death penalty states struggle to obtain lethal drugs, it’s unclear whether fentanyl is the future of death chambers or just a fleeting interest. Will more states switch to opioid-based execution? Or will the course of capital punishment take a different direction?
“It’s Not Like Anyone Thinks This Makes It Less Painful”
Nationally, executions have been on the decline for close to two decades. But last year saw new legal developments and twists in the process. Washington outlawed capital punishment, Alabama witnessed a badly botched execution attempt, Tennessee returned to using the electric chair and Nebraska carried out Moore’s execution, which was the first time fentanyl was used as part of the lethal injection.
Initially, Nevada was slated to be the first state to use the powerful painkiller in its death protocol, for the planned July execution of Scott Dozier. But a last-minute lawsuit halted the procedure after a pharmaceutical company — the maker of one of the other drugs in Nevada’s three-drug cocktail — accused the state of illegitimately acquiring the sedative midazolam. (Dozier later killed himself before the state could execute him.)
For the execution of Moore, the state used a previously untested four-drug cocktail. The protocol first called for a dose of diazepam, which is the generic name for Valium. Executioners followed that with a dose of fentanyl — at which point Moore began coughing and breathing heavily before turning purple, according to the Lincoln Journal-Star. One minute later, Moore was given cisatracurium, a paralytic that would have rendered him unable to breathe. Finally, the protocol ended with a shot of potassium chloride to stop the heart.
All three of the other drugs have previously been used in executions, with some controversy — especially in the case of the cisatracurium, which experts worry could just mask signs of suffering with its paralytic effect.
Supposedly, the fentanyl ensures the condemned is not conscious to feel the effects of the drugs that follow, but Dr. Joel Zivot, an associate professor of anesthesiology at Emory University School of Medicine who has testified as an expert in lethal injection litigation, questions that assumption.
“Having given narcotics to maybe 10,000 or more people in my career, I can’t tell you that everybody gets high or gets pleasure out of it and even the pain relief is uneven,” he told The Fix. “I have certainly never given narcotics and thought, ‘This is going to take away the pain of dying.’ It’s not like anyone thinks this makes it less painful per se to die – it’s unmeasurable and unknowable.”
It may be tempting to think that using a painkiller is a humane final gesture, but Zivot cautions against seeing it that way.
“The Constitution doesn’t ask that you trade off cruelty for being stoned,” he said. “It’s not one or the other, or that being stoned takes away cruelty. It seems like a rather horrible and insensitive way of taking advantage of a terrible national epidemic.”
To death penalty supporters, the opioid’s efficacy in killing — along with the ready abundance of the drug in confiscated supplies — is a selling point.
“Every day people die from this, so it’s obviously effective,” said Houston-based capital punishment advocate Dudley Sharp. “Fentanyl is just an obvious choice. You have unfortunately an inexhaustible supply of this drug in state custody – why can’t it be used?”
“Raised More Questions Than It’s Answered”
Despite the finality of the outcome, some experts say it’s not entirely certain that the first fentanyl execution went as anticipated — because the witnesses couldn’t actually see key parts of the process.
“The Nebraska execution has raised more questions than it’s answered,” said Robert Dunham, executive director of the Death Penalty Information Center. “It isn’t clear that the execution went as planned because the Nebraska prisons dropped the curtain before Carey Dean Moore died, and so none of the witnesses saw the actual death.”
For 14 minutes, witnesses weren’t privy to the goings-on inside the execution chamber.
And given the facial discoloration and signs of “air hunger” before the curtain closed, Dunham said, there’s a possibility the procedure “did not go properly,” a concern that could make fentanyl death protocols less appealing for other states considering the switch.
“Had it been more transparent,” he said, “it might produce a different response from the other states – but the absence of transparency and the questions resulting from that make it unclear whether this was a quote-unquote ‘successful’ execution or just another problematic protocol.”
Because They Could Get It
Even though it’s come to be associated with overdoses, there’s no particular pharmacological reason to start adding fentanyl to death cocktails, according to experts.
“Narcotics are not poison. You can die as a consequence of them,” Zivot said, “but they’re not poison; fentanyl is not made to kill.”
It doesn’t kill better or quicker, and it’s not clear that it does so less painfully. But that’s not necessarily what states are looking for when they pick a new death drug; instead, they’re concerned with availability.
“The way states have selected the drugs is pretty much: they see what other states do and then if it appears to work, they do it too,” Dunham said. “The history of which lethal injection drugs are used can be traced to which ones became unavailable and once drugs became unavailable — because drug companies didn’t want to sell them to prisons for executions — then states began looking for different drugs.”
In recent years, drug companies have refused to provide their products to prisons planning to use them for executions and in some cases, as in Nevada, they’ve even filed suit to ensure their products aren’t used to kill. As a result, some drugs have become harder to get into the death chamber and new combinations have become more appealing.
“When Nevada officials were asked why they chose fentanyl, they essentially said, ‘Because we could get it,’” Dunham said. But even fentanyl could become harder to obtain.
“Eventually with any drug that the drug companies learn is being used in executions,” he continued, “the distribution controls will get progressively stricter.”
But there’s one way to avoid the hurdles of those particular supply-side controls: use something that’s not a drug.
“You Can’t Withhold Nitrogen Gas”
1976: In Room 17 of a seedy Fort Worth motel, a handsome man named Charlie Brooks Jr. stuck a pistol to the face of used car dealer David Gregory.
Six years later, Brooks became the first man in America executed by lethal injection. It was widely touted as a more “humane” way to kill, but the 40-year-old’s death gave pause to that claim.
The four reporters who witnessed it all “appeared shaken by the experience” which “did not appear to be painless,” according to the New York Times.
More than three decades later, the amount of pain condemned prisoners feel is still a source of debate and legal wrangling. It’s made its way into multiple lawsuits over the past year, formed the basis of last-minute appeals and requests for reprieve, and prompted some inmates to beg for alternate methods of execution.
When Doyle Lee Hamm — who survived Alabama’s painfully botched execution attempt early in the year after executioners couldn’t find a suitable vein — sued the state, he cited the bloody procedure as reason not to try again. In June, Houston serial killer Danny Bible unsuccessfully argued that he, like Hamm, was in such bad health that any attempts to execute him could result in a similarly gruesome spectacle. (They did not.) Then in November, Joseph Garcia — one of the notorious “Texas 7” escapees — challenged his pending execution with questions about the safety record of the compounding pharmacy that allegedly supplied the drugs earmarked for his death. The courts refused his last-minute legal claims.
And this winter in Tennessee, death row prisoners begged to die by a different method, ultimately choosing a return to electrocution rather than face the possibility of a botched injection.
These concerns combined with the spread of roadblocks preventing states from getting the drugs they want could be enough to prompt a shift away from lethal injection altogether, some experts believe.
“Lethal injection in the long-term is not viable,” said Sharp. “That’s why a lot of people have been saying to use nitrogen gas because you can’t withhold nitrogen gas.”
In fact, Alabama, Oklahoma, and Mississippi have included nitrogen as part of their execution protocols, though none has actually used it yet. But, experts say, nitrogen might be the next logical option for executions, rather than fentanyl or any other injected drug.
So far, though, it’s an untested procedure.
View the original article at thefix.com